Unnecessary testing in Clinical Laboratory
Unnecessary testing is a common challenge that many clinical laboratories face. The main cause is the absence of processes for extracting and analyzing data of the laboratory’s LIS. Without an analytics system, laboratory staff often rely on time-consuming manual processes. In other cases, laboratories rely on information technology (IT) to compile these reports, which places an additional workload.
An analytics system reduces the need for extraordinary laboratory or IT resources. It also expedites the process of identifying unnecessary testing that the lab carries out. Common categories of unnecessary testing can include tests for screening and diagnosis as well as those for reflex testing.
Examples of unnecessary testing
For instance, when a patient’s level of thyroid stimulating hormone (TSH) is normal, there is no reason to order a test for free thyroxine (FT4) level. This would be an appropriate reflex test in the case of an abnormal TSH level (see Table 1). An example of redundant testing is the simultaneously ordering tests for troponin and creatine-kinase myoglobin (CK-MB). Both of them detect damage to the heart muscle, as in the case of a heart attack. 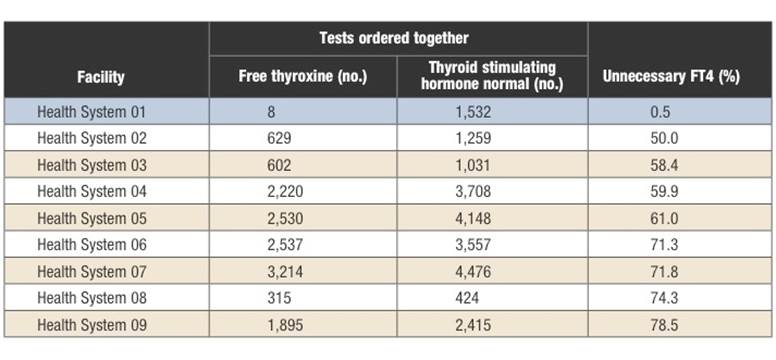
Excessive frequency of repeat testing is also a source of unnecessary testing. For instance, an order of HbA1c testing to determine a patient’s long-term blood glucose level, may take place once every 21 days. Such unnecessary tests represent a drain on the financial resources of the health system. It also present a burden to patients who are undergoing tests unnecessarily. In the table a review of duplicative testing for free thyroxine (FT4) and thyroid stimulating hormone (TSH). One system achieved less than 1% unnecessary FT4 testing. Others reflect unsuccessful implementation of test management strategies (education, CPOE guidelines), or no efforts at all.
An analytics system plays a significant role in managing test utilization. It presents laboratory’s data in a way that identifies unnecessary testing. Additionally it helps lab managers locate the areas of greatest opportunity for corrective action (see Figure 1). Using data of the system, lab managers can establish performance benchmarks. For example the number of tests per inpatient admission, length of stay, and length of stay versus tests per admission. Using such data to create benchmarks enables laboratories to develop an ongoing test utilization program.
Over and under utilization
Both over- and under-utilization of testing have important consequences for patient care and financial performance. In addition to increasing overall costs, overutilization may lead to incorrect diagnoses. It also may lead to waste of time, longer lengths of stay, and even iatrogenic anemia.
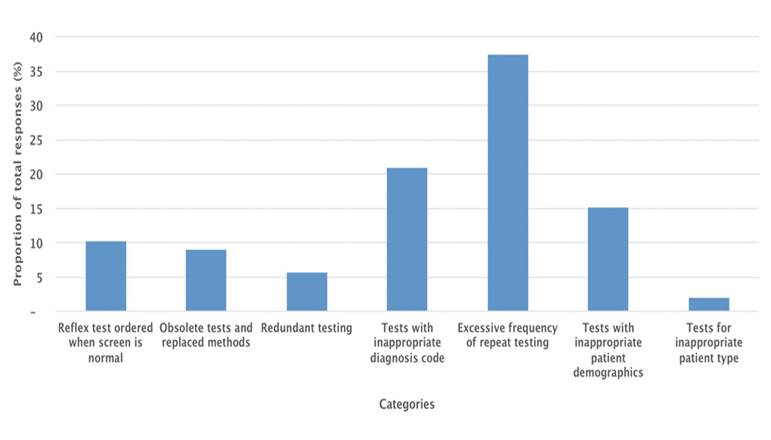
Figure 1. Distribution of categories of unnecessary testing, based on an evaluation of data from more than 100 laboratories.
In cases of underutilization, consequences are significant. These include morbidity due to missed or delayed diagnoses, higher pharmacy costs, and legal liabilities. Studies of malpractice claims show that 48% to 96% of delayed or missed diagnoses resulted from cognitive errors. Common errors are lack of knowledge, mistakes in judgment, and lapses in memory. The most common breakdown was failure to order the appropriate diagnostic test (55% to 58% of cases). Finally, missed and delayed diagnoses harm patients in 48% to 59% of the cases.
By way of example, many health systems are now carefully monitoring admitted patients for sepsis, an inflammatory response to bacterial infection. These can lead to organ failure and death. Health systems that meet the SEP-1 requirements can reduce mortality rates, lengths of stay, and utilization of the intensive care unit. One key element of SEP-1 specifies that if the patient’s lactate level is ≥2 mmol/L, medical staff should repeat the test within 6 hours. Nevertheless, studies show that labs exhibit wide variation in how they observe this particular recommendation.
Using Analytics to improve utilisation
Strategies for Improved Utilization.
To improve test utilization an analytics system provides the necessary meaningful data to identify sources of unnecessary testing. There are a number of strategies that can reduce overutilization of testing. These include the placement of hard and soft stops in the CPOE system. It also includes requisition redesign, test formularies, audits, and education.
With the data from an analytics system, laboratory managers will know the most important areas of unnecessary testing. In that way, the can develope rules for the electronic medical record, providing soft-stop guidance to physicians. In the case of expensive genetic testing, lab managers can block the ordering and referre it to a genetics counselor for approval.
Managers can also use this information to redesign requisitions in order to incorporate professional practice guidelines and limit esoteric tests. For obsolete tests, such as those for creatine kinase isoenzymes, managers may decide to stop offering the test all together. General practitioners may order from a menu of common tests, while specialists order more expensive, esoteric tests. To control unnecessary testing, auditing is the central strategy for addressing underutilization of testing. Without proper auditing, underutilization can go undetected, and in some cases result in serious harm to the patient.
Physician Education.
The auditing functionality enables laboratory managers to monitor the effects of their strategies to manage test utilization over time. Analytics can provide daily performance feedback and an immediate assessment of activities undertaken. Such daily reporting can quickly identify unnecessary testing habits in an organization. This reducess the likelihood that weeks’ or months’ worth of test data may go unchecked.
An analytics system can generate report that provide clear and actionable insight and direction on patterns of unnecessary testing. Such report identify heavy test users and outliers. Using it the organisation can educate physicians about better test ordering practices. For example, monitoring of physician ordering patterns generate reports that identify misinterpretations and unnecessary repeat testing. Use of this may lead to builting rules to support ordering patterns that reduce excessive frequency of testing. For instance the repeat of HbA1c testing within 21 days.
The report may allow a start of a discussion about best practices with the physicians. The goal is to change their habits to align with best practices. It could provide better care for our patients while saving money.
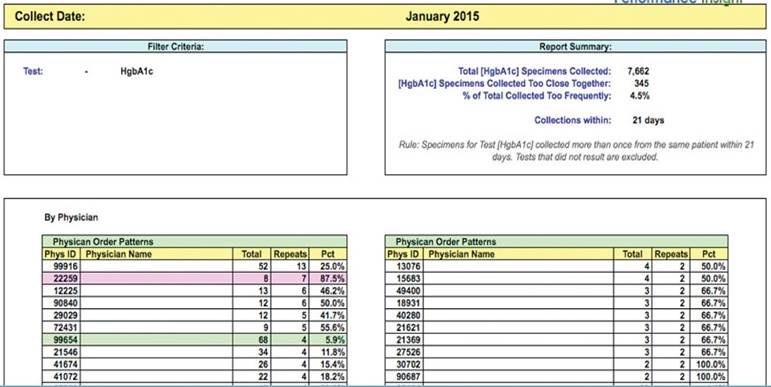
Figure 2. Physician test utilization report, showing excessive frequency of HbA1c testing.
Managing test utilization allows us to monitor correct test ordering as well as appropriate physician testing patterns. Improves standard of care by using this information to educate physicians and other health system members. That way the system flags the Physicians and clinicians that fall short of this standard. After that the organisation uses that information to educate the physicians and to set a standard of care that needs to be followed.
Financial Improvements.
Proper management of test utilization enables health systems to improve their financial performance. An analytics system not only identifies opportunities for immediate cost savings. It can also act longitudinally, enabling laboratory managers to monitor the financial impact of their strategies over time.
Any extent to which laboratories can avoid unnecessary testing represents a contribution to the financial bottom line of the health system. In studies based on audits of client data, we have found that use of an analytics system can result in potential cost savings averaging about $250,000 for every million billable inpatient tests (see Figure 3). For a large health system, that could equate to more than $1 million dollars annually.
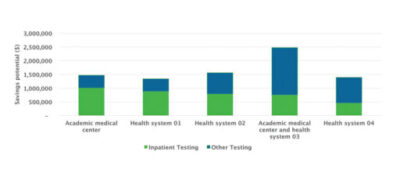 Figure 3. A study identified potential per-lab savings of several hundred thousand dollars annually.
Figure 3. A study identified potential per-lab savings of several hundred thousand dollars annually.
Making the shift
Changes in reimbursement policy are increasingly compelling health systems to pay attention to the test utilization. In turn, managing test utilization requires the development and implementation of best practice protocols. A laboratory analytics system is key to accomplishing this goal. In some respects, these challenges faced by laboratory managers are the same for all laboratories, regardless of size. An analytics system evaluate the Lab’s data and identify the best opportunities for improving test utilization.
In conclusion, to make the best use of the information currently available to a laboratory, a data analytics system often points to the need for a deeper culture shift within the lab. Once this shift is made, laboratories can identify their biggest opportunities to improve test utilization. Laboratory Information System ‘MediLab LIS’ enables hospitals and diagnostic centers of all sizes to focus resources on the best opportunities to improve their bottom line.